
By TLB Contributor:
Please share this important study with as many expectant parents as possible – so they can share it with their healthcare providers. Finally, a government sponsored study that shows that newborns who may be more vulnerable because of low-birth-weight are more at risk for experiencing a variety of immediate adverse events. Do we know what the long-term outcomes will be? With 1 in 68 kids on the autism spectrum and 54% of our kids who are chronically ill – I say it is not hard to figure out.
Although the study refers to low-birth-weight babies… and avoids the term premature births – which are on the rise as excerpted below from an article that came out in March of this year, The United States is the richest country on earth, so why are so many babies born before their time? by Chris Woolston, MS
Premature birth is now the leading cause of death among newborns and a major cause of long-term disability. As reported by the March of Dimes, pre-term births cost the United States more than $26 billion annually. Some babies never recover, but modern medicine gives even the tiniest preemies a fighting chance. Most will eventually go home with their parents, and a good number will have normal, healthy lives. But doctors know this success is clouded by one major failure: Despite their best efforts, they haven’t been able to prevent premature births from happening in the first place.
Why are premature births on the rise, and what can be done to reverse the trend? Siobhan Dolan, M.D., assistant medical director for the March of Dimes, has a short, unsettling answer: Nobody really knows. The factors that can lead to premature birth are extremely complex, she says. One thing is clear: If doctors ever hope to stop this epidemic, they’ll have to understand the forces behind it. Source
Premature births are on the rise because women are more unhealthy at pregnancy. I wrote more on the rise of premature and stillbirths in a blog post not too long ago entitled: Autoimmunity and Stillbirths is there a Connection?
Named a major women’s health issue by the Office of Research on Women’s Health at the National Institutes of Health (NIH), autoimmunity is the underlying cause of more than 100 serious, chronic illnesses. OF the 50 million Americans living and coping with autoimmune disease (AD), more than 75 percent of them are women. ~ Autoimmune Disease in Women
On May 4, ScienceDaily reported that a recent study showed that Premature births can alter the connectivity between key areas of the brain.
The findings should help researchers to better understand why premature birth is linked to a greater risk of neurodevelopmental problems, including autistic spectrum disorders and attention deficit disorders. Source
Finally, studies are finally acknowledging that vaccines can cause damage in subgroups of newborns. How many premature and other at risk babies have been adversely injured in the NICU setting by doctors who feel that they need to be vaccinated on schedule even though they are more vulnerable? It does not even fall into the paradigm of common sense.
If one segment of the infant population has been identified for being high risk for adverse reactions, then we need to identify all others who may be at risk especially since more and more babies are being born with medical issues.
And for all of you who have held on to the crucifix of deception believing that vaccines do not cause injury, this one is for you.
Adverse Events After Routine Immunization of Extremely Low-Birth-Weight Infants
JAMA Pediatr. Published online June 01, 2015. doi:10.1001/jamapediatrics.2015.0418
Importance Immunization of extremely low-birth-weight (ELBW) infants in the neonatal intensive care unit (NICU) is associated with adverse events, including fever and apnea or bradycardia, in the immediate postimmunization period. These adverse events present a diagnostic dilemma for physicians, leading to the potential for immunization delay and sepsis evaluations.
Objective To compare the incidence of sepsis evaluations, need for increased respiratory support, intubation, seizures, and death among immunized ELBW infants in the 3 days before and after immunization.
Design, Setting, and Participants In this multicenter retrospective cohort study, we studied 13 926 ELBW infants born at 28 weeks’ gestation or less who were discharged from January 1, 2007, through December 31, 2012, from 348 NICUs managed by the Pediatrix Medical Group.
Exposures At least one immunization between the ages of 53 and 110 days.
Main Outcomes and Measures Incidence of sepsis evaluations, need for increased respiratory support, intubation, seizures, and death.
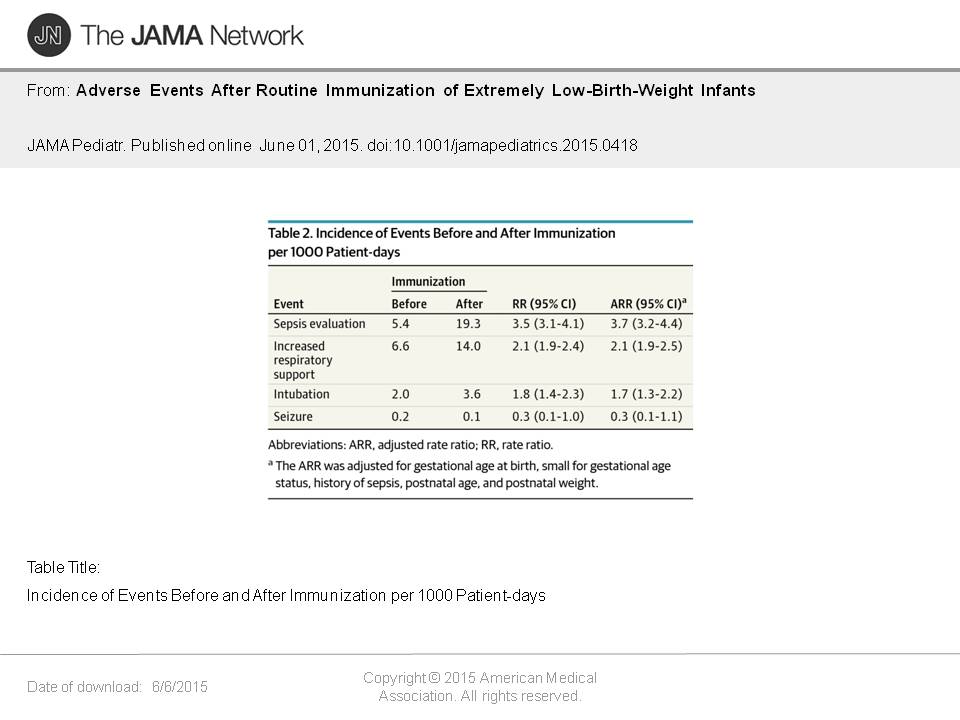
Results Most of the 13 926 infants (91.2%) received 3 or more immunizations. The incidence of sepsis evaluations increased from 5.4 per 1000 patient-days in the preimmunization period to 19.3 per 1000 patient-days in the postimmunization period (adjusted rate ratio [ARR], 3.7; 95% CI, 3.2-4.4). The need for increased respiratory support increased from 6.6 per 1000 patient-days in the preimmunization period to 14.0 per 1000 patient-days in the postimmunization period (ARR, 2.1; 95% CI, 1.9-2.5), and intubation increased from 2.0 per 1000 patient-days to 3.6 per 1000 patient-days (ARR, 1.7; 95% CI, 1.3-2.2). The postimmunization incidence of adverse events was similar across immunization types, including combination vaccines when compared with single-dose vaccines. Infants who were born at 23 to 24 weeks’ gestation had a higher risk of sepsis evaluation and intubation after immunization. A prior history of sepsis was associated with higher risk of sepsis evaluation after immunization.
Conclusions and Relevance All ELBW infants in the NICU had an increased incidence of sepsis evaluations and increased respiratory support and intubation after routine immunization. Our findings provide no evidence to suggest that physicians should not use combination vaccines in ELBW infants. Further studies are needed to determine whether timing or spacing of immunization administrations confers risk for the developing adverse events and whether a prior history of sepsis confers risk for an altered immune response in ELBW infants.
INTRODUCTION
Timely immunization of premature infants in the neonatal intensive care unit (NICU) is associated with improved immunization coverage throughout childhood.1 However, the immunization of extremely low-birth-weight (ELBW; birth weight ≤1000 g) infants has been associated with adverse events, including fever and adverse cardiorespiratory events, such as apnea and bradycardia, in the immediate postimmunization period.2– 4 These adverse events can mimic serious diseases in ELBW infants, including true sepsis, presenting a diagnostic dilemma for physicians. Fever in ELBW infants after immunization can often lead to additional workup to rule out true sepsis, including collection of blood and urine cultures, and exposure to empirical antibiotic therapy. The risks of additional antibiotic use, exposing the infant to painful procedures, and the withholding of enteral feedings must be weighed against the risk of missing true sepsis in an ELBW infant.
Immunization delay has been reported in hospitalized premature infants.5 This delay may be related to physicians waiting to immunize relatively well infants, concerns about adverse events, and misconceptions about the ability of an infant’s immune system to tolerate multiple immunizations.6 Better knowledge of the risk factors for and timing of adverse events after immunization in ELBW infants could lead to better monitoring, prevent unnecessary sepsis evaluations, and reduce immunization delay. To date, most studies describing the incidence of adverse events after immunization in ELBW have been small, single-center studies. In this study, we use a large, multicenter NICU database to investigate the incidence of sepsis evaluations and adverse cardiorespiratory events after immunization in ELBW infants, describe these events by immunization type, and assess potential risk factors for adverse events. Read more here.
RESULTS
We identified a total of 13 926 infants who received a total of 48 853 immunizations (Table 1); 12 703 infants (91.2%) received 3 or more immunizations. The median postnatal age at immunization was 64 days (interquartile range, 60-72 days). A history of sepsis before day 53 was observed in 2904 infants (20.9%). During the preimmunization and postimmunization periods, 5952 (42.7%) of 13 926 infants received caffeine therapy.
There were 5 deaths in the postimmunization period. Three of the 5 infants who died in the 3 days after immunization had a diagnosis associated with death available in the data set; 1 infant had a bowel perforation, 1 infant had necrotizing enterocolitis and presumed sepsis, and 1 infant had pneumonia and respiratory failure. The incidence of sepsis evaluations, increased respiratory support, and intubations measured by day, from 30 days before immunization to 30 days after immunization, revealed a steady decrease until 5 to 7 days before immunization, followed by a sharp decrease leading up to the day of immunization (Figure). After immunization, there was an increase in the daily incidence between day 0 and day 2 after immunization, most notably for sepsis evaluations (Figure). When analyzing adverse events grouped by type of immunization administered, we found pneumococcal conjugate to be the most commonly administered immunization (Table 3). The incidence of adverse events was similar across all immunization types, with the primary outcome (sepsis evaluation) again revealing a higher postimmunization incidence across all types of immunizations (Table 3). Read more here….
CONCLUSIONS
This study found an increase in adverse events after the routine immunization of ELBW infants in the NICU, specifically sepsis evaluations, need for increased respiratory support, and intubation. The incidence of these adverse events decreased sharply just before the first immunization day. Younger gestational age (23-24 weeks) was associated with a higher risk of sepsis evaluation and intubation after immunization. A prior history of sepsis was associated with a higher risk of sepsis evaluations after immunization. Further studies are needed to determine whether the order and timing of specific immunizations affect the incidence of adverse events in the postimmunization period and whether a prior history of sepsis confers risk for an altered immune response in ELBW infants.
ARTICLE INFORMATION
Conflict of Interest Disclosures: Dr Smith reported receiving consulting fees from industry for neonatal and pediatric drug development (https://www.dcri.org/about-us/conflict-of-interest/). No other disclosures were reported.
Funding/Support: This study was supported in part by grant 1R18AE000028-01 from the US Department of Health and Human Services (statistical support), award UL1TR001117 from the National Center for Advancing Translational Sciences of the National Institutes of Health (research support), and grants HHSN267200700051C, HHSN275201000003I, and UL1TR001117 from the National Institutes of Health and the National Center for Advancing Translational Sciences of the National Institutes of Health (salary support) (Dr Smith).
Role of the Funder/Sponsor: The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and the decision to submit the manuscript for publication.
Disclaimer: The content of this article is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
****************
Leslie Carol Botha is an Author, publisher, TLB radio talk show host and internationally recognized expert on women’s hormone cycles. Social/political activist on Gardasil the HPV vaccine for adolescent girls. Co-author of “Understanding Your Mood, Mind and Hormone Cycle.” Honorary advisory board member for the Foundation for the Study of Cycles and member of the Society for Menstrual Cycle Research.
****************
TLB recommends you visit Leslie at Holy Hormones Journal for more pertinent articles and information.


Leave a Reply